












          |
   |
|
|
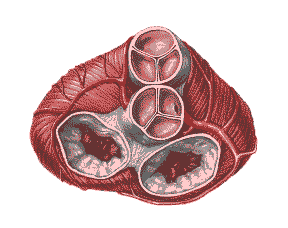
A cross–section of the heart showing the aortic valve, mitral valve, tricuspid valve and pulmonary valve. |
Approximately 70,000 heart valve replacement procedures are performed annually in the United States for conditions ranging from Mitral Valve Stenosis resulting from rheumatic fever, Mitral Regurgitation from "floppy" valves, and Calcified Aortic Stenosis encountered in large numbers of aging patients, particularly elderly women.
Mitral valve stenosis occurs predominantly in women. The reasons for this are unknown but it has been documented in virtually every clinical series about the disease since the turn of the century.
The incidence of rheumatic disease has markedly decreased in the United States due to better prophylaxis treatment of streptococcal infections with the use of antibiotics. Paradoxically, the treatment of mitral valve stenosis may be increasing. The reasons are related to immigration and the incidence of rheumatic heart disease in third-world countries. Immigrants from southeast Asia and South and Central America currently comprise a large number of patients in the United States with rheumatic heart disease.
Mitral valve regurgitation (also referred to as mitral valve prolapse or MVP) follows a very different path for a woman versus a man. The condition of mitral valve prolapse is commonly diagnosed in young females yet the incidence in elderly women decreases markedly. Conversely, there is a fairly consistent incidence of mitral prolapse in the male population at both young and old age. Recent studies have indicated that, for men, the incidence of mitral prolapse requiring surgical intervention is higher than for women and it increases with age (Wilcken DEL, HickeyAJ Liftime: Risk for patients with mitral valve prolapse of developing severe valve regurgitation requiring surgery. Circulation 78:10-14, 1988). There is much interest in the etiology of mitral regurgitation. Once the diagnosis of MVP is confirmed, it requires constant vigilance against endocarditis, arrhythmia and mitral regurgitation.
Obtaining medical insurance after being diagnosed with MVP may be difficult for a woman as there is important stigmata associated with the diagnosis, however, there is little evidence that MVP bears a serious prognosis in young women. A research initiative over a 10-year period could provide definitive longitudinal information that may help remove the stigma of the diagnosis for medical insurance purposes.
The most common acquired lesion in the practice of adult cardiac medicine is calcific aortic valve disease with aortic stenosis. Greater confidence in the success rate of open heart procedures in the elderly has led to more valve surgery and coronary bypass operations being performed on those with calcific aortic valve disease. Survival rates are similar for both women and men over age 70 having valve surgery, with or without coronary bypass (for treatment of vessel disease). Issues surrounding quality of life and cognitive functioning need to be assessed with longitudinal studies to determine proper use of resources. Randomized prospective studies would be helpful to better define risk in the elderly.
The choice of a cardiac valve is very complex and involves a number of socioeconomic, physical, cardiac and gender-related factors. Age, mental status, risk factors for bleeding and cultural beliefs are all taken into consideration. Most important is how to manage mitral valve disease in a woman in the prime of her reproductive years or, rarely, in a pregnant patient who has a severe exacerbation of mitral valve disease and needs a surgical operation.
One surgical treatment for mitral valve stenosis that does not involve open heart surgery is transfemoral mitral valve balloon angioplasty. This procedure has been used successfully in third-world countries but is just starting to be used in the United States. It may be the treatment of choice for noncalcific fibrotic mitral stenosis. It may also be most applicable in young women, though there are no controlled, randomized prospective studies of open mitral commissurotomy versus closed mitral commissurotomy. More research is needed in this area.
Pregnant women with exacerbation of mitral valve disease and who require surgery may want to consider the transfemoral mitral valve balloon angioplasty. This is an excellent choice as these women are usually without calicified valves with fibrotic commisures. While open heart valvuloplasty can be done during pregnancy, there is increased risk to the fetus the longer the mother is on cardiopulmonary bypass.
The best option for valve surgery is to have valve repair. It allows the patient to avoid long-term anticoagulation therapy and leaves the anatomy of the heart muscle unchanged. It allows women of child-bearing age to plan a pregnancy. Nothing is as efficient as the human body. Most patients at major valve surgery centers now undergo mitral valve reparative procedures rather than valve replacement. This trend toward surgical repair has caused a change in the indications for mitral valve surgery for this disorder, since both prosthetic and bio-prosthetic valves have characteristic "natural" histories. In North America, the vast majority of patients who undergo mitral valve repair have prolapse of the mitral valve (floppy valve) or mitral regurgitation related to ischemia (local and temporary anemia due to an obstruction of blood flow to the heart).
Not everyone is a candidate for valve repair. If having a valve replacement, there are two types of artificial valves to choose from...
For prosthetic valves, the main risk is blood clot formation (thromboembolism) or hemorrhage secondary to anticoagulation therapy. For bioprosthetic valves (porcine, pericardial), the main risk is structural valve degeneration and re-operation. Repair of the mitral valve rather than replacement with a prosthetic valve is the best choice as it allows maintenance of the normal heart muscle and preserves function, improving both early and late survival by maintaining the normal shape of the left ventricle.
What is the best artificial valve to replace the mitral valve in a woman? The mechanical valve has the advantage of the longest durability and the lowest probability of re-operation, however, because of the nature of the prosthetic material in mechanical valves, long-term anticoagulation with warfarin is an absolute necessity. Without it, there is a high probability of thromboembolism to the brain and other organ systems. Therefore, the mechanical valve should not be used in women who are pregnant or who have reproductive capability.
The first mechanical valve was produced decades ago and there have been enormous changes over the years. The mechanical valve that is implanted today is made of pyrolytic carbon and titanium. There are various manufacturers, styles and sizes. It was made to last forever, but it requires anticoagulation for the patient’s lifetime. Some patients may feel that anticoagulation management is overwhelming, but each person should be made aware that, once a routine dose has been established, a once-a-month blood draw at a local outpatient lab facility is usually all that is required, along with being alert to signs of bleeding.
Complications associated with mechanical valves center around anticoagulation therapy. If the blood is too “thin”, the patient can experience bleeding. If the blood is too “thick’, it can cause clots to form on the new valve, laying the foundation for catastrophic problems. However, if the biggest problem is closely monitoring the blood to prevent complications, a solution is now available. Home monitoring units allow a patient to do a finger stick to check her own blood levels just as a diabetic patient monitors her own blood sugar. This allows the patient to have a significant role in her recovery and health maintenance with very little disruption of her routine. Patients are able to tightly control their blood levels and monitor their blood at any time. And, they can travel without scheduling their lives around their blood draws. Self-monitoring makes the choice of a mechanical valve more appealing for some. Some cardiac surgery centers provide patients who have had a mechanical valve implanted with this self-monitoring unit and also provide the educational follow-up to promote independence.
There are several manufacturers, styles and sizes of tissue valves. The tissue valve is commonly a “porcine” (pig) or “bovine” (cow) and on occasion a “homograft” (human) valve. These valves offer lifestyle advantages over mechanical heart valves in that patients do not usually need the lifelong anticoagulant therapy required with mechanical valves. This benefit makes the tissue valve appropriate for older patients and women of childbearing age, as well as patients who may live in areas where close physician monitoring of their anticoagulation regimen is difficult.
Bio-prosthetic valves can be implanted without need for long-term anticoagulation in the young patient in sinus rhythm but have an uncertain durability that will inevitably require re-operation. This may occur at any time from 5 to 15 years postoperatively. While the patient is not subjected to the complications associated with anticoagulation, if the valve “wears out” then the patient must endure re-operation with valve replacement -a risky procedure.
If you are one of the 70,000 patients requiring heart valve surgery each year, use this informational page as a starting point to discuss with your doctor the treatment approach that is best for you.
1. Derived from Proceedings of an NHLBI Conference: Cardiovascular Health and Disease in Women: "Valvular Heart
Disease" by Cohn, L, MD. Chap52, p335- 339. Editors: Nanette K. Wenger, MD, L.
Speroff, MD, B. Packard, MD, PhD., copyright 1993, Le Jacq Communications publishing company.
2.Union Memorial Hospital Department of Open Heart Surgery, Baltimore, MD.
Graphics courtesy of Union Memorial Hospital
State Report Cards | Questons Before Heart Surgery | Heart Surgery Options | Scarless Heart Surgery | Valve Surgery Options | Bloodless Care: What You Need to Know | Being Informed About Your Medical Care
Disclaimer | Donate Now | Contact Us | Site Map | Store
|
©1999-2000; updates: 2002, 2004, 2005, 2007 Women's Heart Foundation, Inc. All rights reserved. Unauthorized use prohibited. The information contained in this Women's Heart Foundation (WHF) Web site is not a substitute for medical advice or treatment, and WHF recommends consultation with your doctor or health care professional. |