












          |
   |
Mitral valve prolapse (MVP) is the most common condition of the heart valves. Some studies show it affects 6% of all women.
Incidence
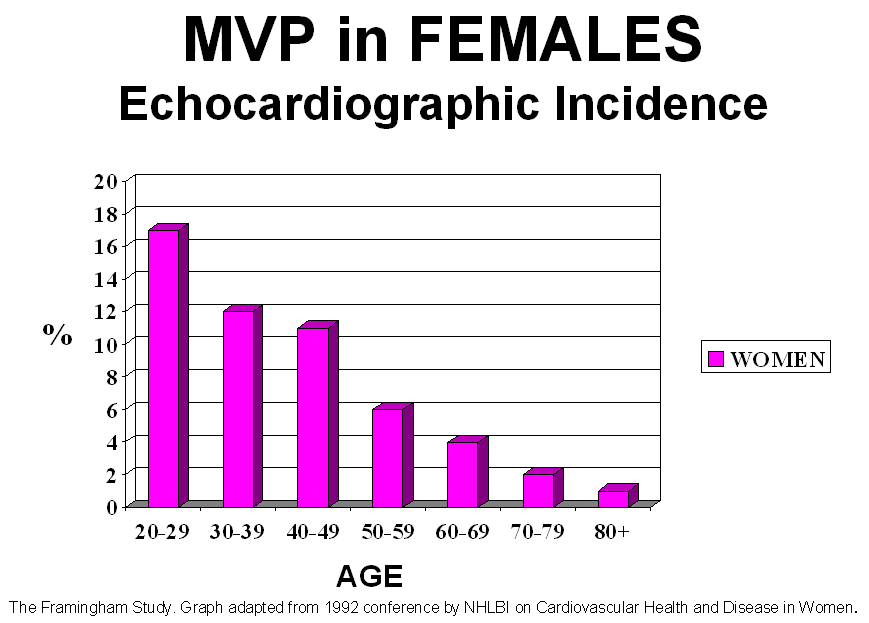
MVP is extremely interesting since it is so commonly diagnosed in
young women and yet, the incidence decreases markedly in elder women.
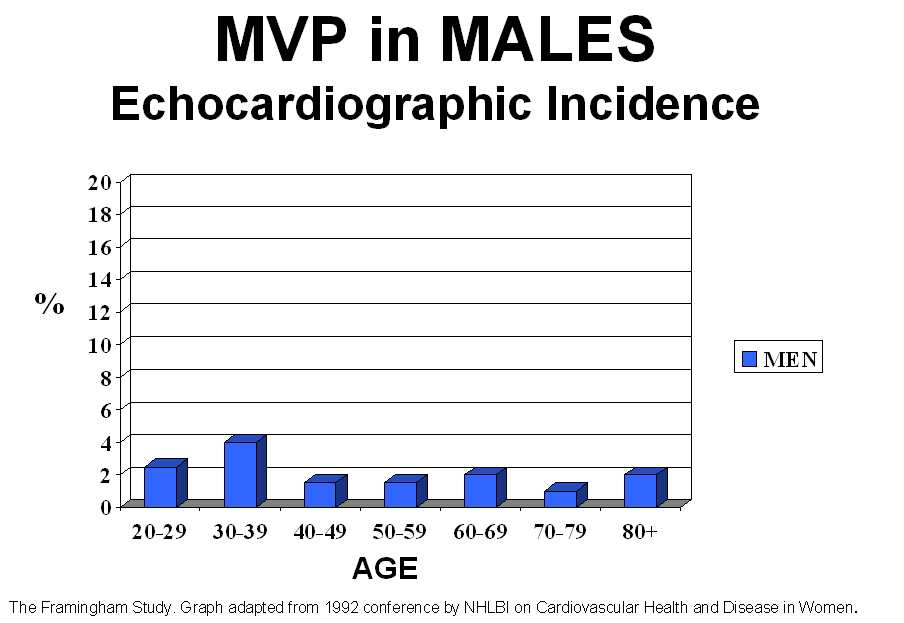
This drop off in incidence is not seen in the male population
(refer to graph below).
The occurrence of MVP in men is consistent in both young
and old populations. Previous to the Framingham study, the incidence of
MVP was thought to be much higher in women, however, with this new data,
it is now believed that MVP affects equal numbers
of men and women. This intrigues researchers searching
for the cause(s) of mitral valve disease and attempting to explain
why the condition
manifests itself so differently in men and women.
The cause of MVP is usually unknown but occassionally, MVP is associated with other heart conditions (e.g. atrial septal defect, coronary artery disease, diseases of the heart muscle) but most likely, these diseases would have been present with or without MVP.
The outcome from MVP differs for men and women too. Recent studies have indicated that, for men, the incidence of mitral prolapse requiring surgical intervention is higher than for women and increases with age.
The two graphs below depict the differences in the incidence of mitral valve
prolapse in men and women. As the graphs indicate,
the incidence remains rather consistent in the male population. Contrastly,
occurence starts off high in females, then sharply declines in older women.
Data is derived from the Framingham study.
What is the mitral valve?
The mitral valve is one of four heart valves. It is located
between the left atrium of the heart, which receives fresh, oxygenated
blood from the lungs, and the left ventricle, which pumps the blood
out to the body. The mitral valve receives its name due to its
shape, which resemble a bishop's miter with two peaks. The graphic below
shows the location of the mitral valve and the blood flow through the
chambers of the heart when there is mitral valve regurgitation or
back flow of blood in the left ventricle.
|
The mitral valve has two flaps or leaflets. They are shaped somewhat like a parachute and are attached to supporting muscle by strings. Normally, by opening and closing, the blood is allowed to flow in only one direction –– from the left atrium to the left ventricle. In mitral valve prolapse, this may not be true.
The American Heart Association describes mitral valve prolapse as “(when) one or both flaps (of the mitral valve) are enlarged and some of their supporting strings are too long. So, when the heart contracts or pumps, the mitral valve flaps do not close smoothly or evenly. Instead, part of one or both flaps collapse backward into the left atrium. This sometimes allows a small amount of blood to leak backward through the valve”.
Other names for MVP are the “Click–Murmur Syndrome”, “Barlow's Syndrome”, “Click Chick”, “Straight Back Syndrome”, “Balloon Mitral Valve” and “Floppy Valve Syndrome”.
How is MVP diagnosed?
MVP is diagnosed most often by your doctor when listening to your heart with a stethoscope and hearing an extra click or murmur. It is confirmed through echocardiogram – a non– invasive test using sound waves to “see” inside the heart.
Symptoms from MVP vary from having no symptoms, mild symptoms and many symptoms. About 60% of people that have MVP don't even know they have it because they have no symptoms.
Symptoms include palpitations, shortness of breath on exertion, chest pain that comes and goes for no apparent reason, panic attacks, unexplained fatigue and migraine headaches. These symptoms can adversely affect quality of life and should be addressed by your attending physician or practitioner. He/she may advise that you start a regular exercise program and cut down on your caffeine intake, decongestant use or other drugs that can trigger rapid heartbeat. Your practitioner may also advise that you wear a Holter monitor – a device that records your electrocardiogram for 24 hours (other devices are available to wear for up to several weeks of monitoring).
What is the treatment for MVP?
The majority of MVP patients who have no symptoms will need no treatment but, for those diagnosed with MVP with echocardiogram showing some significant leakage across the valve, one must always be vigilant against endocarditis,(inflammation of the heart muscle), arrhythmia and mitral regurgitation. MVP makes one susceptible to bacterial infection (from strep, for example). Strep is introduced during dental work or certain surgical procedures. Those with leaky or regurgitant prolapsing valves will need antibiotics to prevent infection of the valve during certain surgical procedures likely to cause bleeding. Typically, this involves taking two doses of an antibiotic– one an hour or two before the procedure and another six hours after the first, according to the AHA. In a small number of MVP patients with chest pain or abnormal heart rhythms, medicine may be used.
In closing, mitral valve prolapse is a condtion that should be monitored by your doctor, but it should not prevent you from having a full and active life.
Sources:
Amercan Heart Association
Cohn, Lawrence H., MD, Proceedings of an NHLBI Conference on Cardiovascular Health
and Disease in Women, Chapter 52: Valvular Heart Disease, P335-339.
Rosenfeld, I, MD, “If There's a ‘Click’in Your Heartbeat”, Parade
Magazine, Jun25,'00
Image of Mitral Valve Prolapse used by permission.
Alcohol and Heart Disease |
Gender Differences |
Mitral Valve Prolapse |
Women’s Heart Risk Quiz
Sleep Disturbances: Heart at Risk |
What is Heart Disease? |
Cardiac Arrhythmia Management in Women |
Heart Disease Facts |
Panic Attack or Heart Attack |
Three Women from New Jersey
|
Noreen
|
Disclaimer | Donate Now | Contact Us | Site Map | Store ©1999-2000; updates: 2002, 2004, 2005, 2007 Women's Heart Foundation, Inc. All rights reserved.
Unauthorized use prohibited. The information contained in this Women's
Heart Foundation (WHF) Web site is not a substitute for medical advice or
treatment, and WHF recommends consultation with your doctor or health care
professional.